What exactly is Infection Control?
Infection Control is a way to minimize the transmission of microbes in the dental office. Potentially, diseases could be transmitted in a dental setting in three ways - from patient to dental-care provider, from patient to patient, and from dental-care provider to patient. Infection control procedures arrests transmission of diseases by using different methods such as - physical barriers, chemical agents, and heat.
- Is it safe to Go to the Dental Office?
- Why Is the Dental Team Concerned About Infection Control?
- Dentistry's leadership in infection Control
- How are Infectious Diseases Transmitted?
- What Exactly Is Infection Control?
- Universal Precautions
- Everyone Benifets from Infection Control
- Who sets Infection Control Guidelines ?
- How is infection control Implemented?
- What are the Infection Control Procedures ?
- What Does the Dental Team wear?
- What is Disinfection?
- What is sterilization?
- Do all dental instruments need to be sterilized?
- Is there a way to be sure that sterilization has worked?
- Can Dental Handpieces Transmit Infection?
- Where does the Infectious waste go?
- What about AIDS?
- The Controversy
- YES, IT IS SAFE to go to Dental Office
- What do we, at Agoka Dental, do to keep our Dental Office Safe?
Is it safe to Go to the Dental Office?
Yes, This section describes the many measures, the behind-the scenes activities, that we, at Agoka Dental, undertake to ensure that you are not exposed to disease-causing microbes (germs) in our dental office. These measures have been developed over the years in response to concerns about the possibility of transmitting or contracting diseases, particularly hepatitis and HIV, in various health-care settings. The measures are many, and vary from the simple - such as hand washing or the disinfection of a countertop - to the elaborate, such as the sterilization of instruments with high-pressure steam.
Be assured that your dental office has never been more safer.
back to top
Why Is the Dental Team Concerned About Infection Control?
Members of our dental team care very much about your well-being and health. Dental-care providers abide by a code of ethics established by the American Dental Association. This code of ethics has, as its primary goal, your safety. Dating back to Hippocrates, this imperative of health-care providers declares, "Do no harm." Abiding by these ethics helps guarantee quality care while minimizing any associated risks.
Infection-control procedures are one way of caring for both you and the dental team by minimizing the risk of transmission of pathogens (disease-causing microbes, or germs) from dental-care provider to patient and patient to dental-care provider.
Our dental team puts forth considerable efforts in preparing the dental operatory for individual patients; most of this preparation is accomplished long before you are seated in the dental chair.
back to top
Dentistry's Leadership in Infection Control
Studies have shown that dentists are in fact more willing and accommodating in practicing infection-control techniques than other health-care providers.
back to top
How Are Infectious Diseases Transmitted?
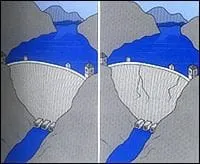
1. The person exposed to the infectious microbes must be susceptible. A variety of factors influence susceptibility, including general state of health, and previous infections or immunizations, which sometimes results in the creation of protective antibodies. For instance, individuals successfully immunized against the hepatitis B virus are no longer susceptible to infection by this virus.
When germs become too numerous, they overwhelm the body's defenses, like water breaking through a dam
2. A specific number of infectious pathogens must be present. The body's immune system can usually resist a limited number of microbes, but if the microbes become too numerous, they overwhelm the body's defenses and cause an infection.
3. The microbes must be highly infectious. Weakened viruses can actually be put to use; many vaccines consist of weakened viruses that do not cause disease but instead enable the body to form protective proteins - antibodies - that make individuals immune to disease.
4. Pathogens must enter the body in an appropriate manner. Depending on the microbe and where it enters the body, infection may or may or occur. For instance, if HIV enters the mouth, infection will most probably not occur. But if it enter the blood stream directly, an infection will probably occur.
Infection-control procedures are designed to disrupt these four conditions, reducing the possibility of disease transmission dramatically.
back to top
What Exactly Is Infection Control?
Infection control is a way to minimize the transmission of microbes in the dental office. Potentially, diseases could be transmitted in a dental setting in three ways-from patient to dental-care provider, from patient to patient, and from dental-care provider to patient.
Infection-control procedures arrest disease transmission by using different methods-such as physical barriers, chemical agent, and heat.
back to top
Universal Precautions

back to top
Everyone Benefits from Infection Control
Many people don't know that the dental-care providers are at higher risk of contracting infectious disease from their patients than are patients from dental-care providers. However, since the introduction of universal precaution and recommendation for vaccination against pathogens such as the hepatitisB virus, the rate of infectious diseases acquired by health-care provider has decreased dramatically.
Federal and state government have laws and regulations that require employers to provide safe workplace conditions for every employee. These laws and regulations require employers to provide employees with appropriate protection against infection. These infection-control procedures benefit both you and members of the dental team.
back to top
Who Sets Infection Control Guidelines?

Professional organizations, such as the American Dental Association (ADA), issue infection-control guideline for dentists. These recommendations are revised and updated continually by world leaders in the field of infection control.
back to top
How Is Infection Control Implemented?

A dentist prepares the treatment area for a patient
1. Using physical barriers for protection. In the dental office, you might see chair covers or other protective devices, such as masks, gloves, eye wear, or disposable gowns. These physical barriers are for your benefit, as well as for the protection of the dental team. These barriers are changed between patients.
2. Using disposable items. In addition to the disposable physical barriers, dentists use, as much as possible, disposable bibs, disposable cups, and disposable saliva ejectors (suction tips). Such items help minimize the spread of infection.
3. Cleaning instruments and equipment thoroughly between patients. This involves destroying or reducing the number of microbes that have contaminated dental equipment that is not disposable. The dental team also takes extra care to practice clean work methods.
4. Attempting to identify as many patients as possible who are infectious. This also enables the referrals of patients for appropriate medical care. Furthermore, certain infectious conditions may warrant a change of dental procedures.

Because many people see their dentist more frequently than their physician, dentists are in a good position (and even feel obligated) to identify possible medical conditions. Helping you identify any such conditions is the first step toward ensuring that you are getting the care you need.
back to top
What Are the Infection-Control Procedures?
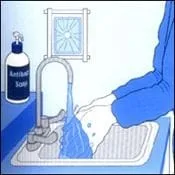
Asepsis
Asepsis is the first way to prevent contamination. In asepsis, microbes are not necessarily destroyed, but their ability to infect is interrupted. In dentistry, asepsis is achieved in two ways.
1. Hand washing. The dental team washes their hands before and after every patient.
2. Barriers and coverings. Physical barriers, such as gloves, gowns, masks, and disposable coverings placed in items such as switches and controls, prevent the possibility of contamination.
back to top
What Does the Dental Team wear...?
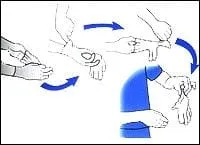
Gloves
Gloves are worn to prevent exposing the dental-care provider's skin to the microbes in blood, saliva, or mucous membranes. Gloves are changed between patients, and dental team members wash their hands, both before putting on their gloves and after removing them. Some prefer to wear sterile gloves or surgical gloves for certain procedures, as well as regular vinyl gloves. Latex gloves, known as examination gloves, are appropriate for all general dental procedures and are most commonly used.
Infection control guidelines even address the way gloves are put on, take off, and disposed of.
Masks

Masks also protect the patient from exposure to upper respiratory-tract pathogens that a member of the dental team may be harboring.
Glasses
Protective eye wear, in the form glasses with side shields, or a face shield, is used to protect the eyes from blood, saliva splatters, and dental aerosol. In some dental offices, patients are also asked to wear protective eye wear to minimize the chance of physical injury to their eyes during certain dental procedures.
Gowns
Members of the dental team wear gowns during procedures that generate dental aerosol. These gowns are usually fluid-resistant and act as a physical barrier to prevent exposure from aerosols and other matter to street clothes and bare skin. These gowns can be changed between patients or when visibly soiled. Many dental offices employ outside contractors to clean and prepare non disposable gowns before they are used with patients.
back to top
What Is Disinfection?

Many types of disinfectants are available, but we, at Agoka Dental, usually choose products registered with the Environmental Protection Agency (EPA) and approved by the American Dental Association (ADA). All disinfectants used in our dental office are designed to destroy even very resistant bacteria, such as M. tuberculosis. Premixed disinfection solutions are changed on a regular basis, as determined by their expiration date, to assure maximum effectiveness.
back to top
What Is Sterilization?

An item can be sterilized in a number of ways. Commonly, instruments are treated with high-pressure steam for an extended period of time. This process is known as autoclaving.
Autoclaving process

In autoclaving, instruments (which are first cleaned, dried, and placed in a special steam-penetrable wrap), are subjected to pressurized steam for 15 to 20 minutes. The machine that performs this process is called an autoclave. After autoclaving, the instruments are left in their protective packaging until they are ready to be used in the treatment of a patient.
Cold Sterilization
For items that would be damaged by the high heat involved in other sterilization processes, a nonheated liquid sterilization procedure is used. This involves soaking the contaminated object in a chemical solution, such as glutaraldehyde, for about 10 hours.
back to top
Is There a Way to Be Sure That Sterilization Has Worked?
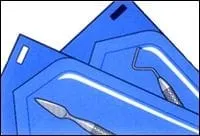
Chemical monitoring is accomplished with the use of a special ink. A strip of heat-sensitive ink is included in the package with the instruments during the sterilization process. The ink changes color when the required temperature has been reached. This ink change then signals to the dental team that packaged instruments have been exposed to the proper temperature.
Biological spore testing is done by testing the sterilization process on harmless live bacteria, which are contained in sealed vials. Biological spore monitoring is considered a more reliable method of measuring the effectiveness of sterilization. It is accomplished by exposing difficult-to-destroy bacteria to the normal sterilization process and verifying that these bacteria have in fact been destroyed. If sterilization was not successful, the instruments are not used on patients and the sterilizer is repaired or replaced.
back to top
Can Dental Handpieces Transmit Infection?
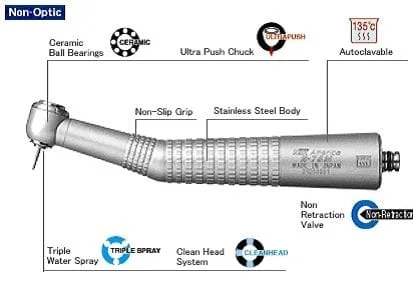
"We, at Agoka Dental, use high speed handpieces that have anti-retraction valve built into the handpiece. They also have a patented 'Clean Head System' that prevents or reduces the debris from entering the Handpiece. Hey, we treat our own children here; we better be very careful."
back to top
Can Dental Handpieces Transmit Infection?
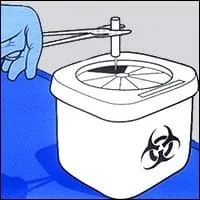
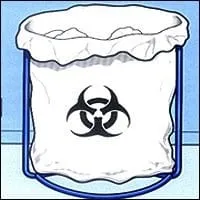
Burs and other sharp disposable materials that may be used in the course of dental procedures have special containers for disposal. These "sharps" are placed in designated containers that are puncture resistant, leakproof, and specially labeled. Like other infectious waste, their disposal is governed by various regulations.
back to top
What About AIDS ?
Transmission of HIV occurs through contact with blood, intimate sexual contact, and from HIV-infected mothers to their newborns. Casual contact has never been known to transmit HIV. HIV cannot be transmitted by tears, urine, sweat, dental aerosol, or insect bites. Furthermore, HIV is a very fragile virus-it is easily killed by disinfectants regularly used in dental offices.
Recent studies have suggested that saliva contains components that render HIV harmless. In fact, these factors that inhibit HIV are being widely studied and one day may be used to treat HIV disease.
HIV has not been shown to be transmitted even when blood is present in saliva. Thus, being a patient in a dental office that treats HIV-infected patients does not pose any risk. However, even if there were a chance that HIV could be transmitted in a dental office, adherence to "universal precaution" would virtually eliminate such an occurrence. Furthermore, it is probably safe to presume that dental offices that knowingly treat HIV-infected patients will have the best infection control available!
back to top
The Controversy
Since the initial reports of HIV- infected patient in the early 1980s, the possible transmission of HIV in health-care setting has been debated both among health-care providers and in the lay press. Concern heightened in 1990, when CDC, the federal watchdog agency for public health policy, reported a possible transmission of HIV from a dentist with AIDS to one of his patients. Since that time, five additional patients have come forward claiming to have been infected by the same dentist.
Numerous investigations have tried to explain if and how such a transmission might have occurred, but none have succeeded in doing so. Furthermore, even today, this case remains a puzzle, as no mode of transmission has been detected and no other cases have been found where HIV-infected health-care providers have been implicated in the transmission of HIV to patients. In fact, the opposite seems to be true. Studies of over 22,000 patients treated by 51 HIV-infected health-care providers, 29 of them dentists and dental students, could not document a single case of HIV transmission from an infected health-care provider to a patient.
Because HIV is so fragile, and because all equipment and surfaces that may have been contaminated are cleaned and disinfected between each and every patient, it's not surprising that HIV transmission between patients has never been documented in a dental office.
back to top
YES, IT IS SAFE to go to Dental Office
Yes! You now know that all dental equipment is replaced, disinfected, or sterilized between patients. In some cases, additional protective barriers are used to facilitate cleaning. You may notice plastic or latex wraps or aluminum foil on the light handles or covering the chair controls in the dental office. All of these measures are ways of ensuring your safety in the dental setting.
Dental offices that use appropriate infection-control techniques and routinely practice "universal precaution" for all dental procedures are safe. The members of the dental team care very much about your safety and follow every known recommendation to prevent the transmission of disease in the dental setting.
Because of the increasing sophistication of infection-control measures, your dental office has never been more safer.
back to top
What do we, at Agoka Dental, do to keep our Dental Office Safe?
- Employ "Universal Precautions" for all of our patients.
- Use and review the health history form of all of our patients.
- Immunize ourselves and all staff against hepatitis B.
- Follow OSHA / ADAA / CDC recommendations and guidelines.
- Regularly attend infection-control update courses and integrate new practices into the dental office.
- Use protective barriers such as glasses, gloves, masks, and gowns.
- Disinfect patients treatment area before each patient.
- Sterilize the dental instruments and handpieces.
- Monitor disinfection and sterilization solution for efficacy.
- Monitor sterilizers for efficacy.
- Dispose of infectious waste according to federal, state, and local law.

